
Alexander McLawhorn, MD, and his team understand how debilitating knee arthritis can be. That's why our state-of-the-art facility offers a comprehensive approach to diagnosing and treating knee pain and other arthritis symptoms.
With a wealth of expertise in the latest medical advancements, we provide innovative solutions to enhance mobility and relieve pain. Discover the path to optimized knee health and regain the freedom to move with confidence.
Knee arthritis can profoundly impact your quality of life, manifesting as persistent pain, stiffness, and reduced mobility that interfere with everyday activities. Whether it's the challenge of climbing stairs, the discomfort of standing from a seated position, or the relentless ache after a day's activities, the symptoms can be debilitating.
Fortunately, help is at hand. Dr. Alexander S. McLawhorn, a distinguished orthopedic surgeon at Hospital for Special Surgery, offers expert diagnosis and treatment plans in New York City and Stamford, Connecticut. Dr. McLawhorn will help find ways to alleviate your pain and restore mobility, so you can get back to the activities you love..
What Is Knee Arthritis?
Arthritis is characterized by damage to the joint surfaces where they make contact with one another. In the knee, arthritis impacts the ends of the femur (thigh bone), tibia (shin bone), and patella (kneecap).
In healthy knees, the surfaces of the knee joint are surrounded by a protective covering of cartilage. When cartilage breaks down due to injury, aging, normal wear and tear, or other conditions, the bones can begin to rub directly together. The normal joint space between the bones narrows, and bone spurs (osteophytes) and cysts can form. Invariably, the menisci are also damaged and can tear as a part of the arthritic process. When the damage to the joint becomes severe, the ligaments around the knee can be affected, too.
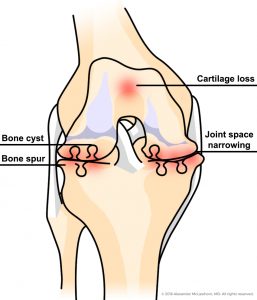
Knee arthritis causes joint pain, stiffness, and immobility. With very severe arthritis, the leg may develop bowing ( also known as a “varus” deformity) or become “knock-kneed” (also known as a “valgus” deformity), and patients may feel the knee is unstable once the ligaments are damaged.
What Are the Different Types of Knee Arthritis?
There are several different types of knee arthritis that can all lead to destruction and deformity of the knee joint.
Though the symptoms associated with arthritis in the knee may be similar regardless of the type of arthritis, the reasons for developing the disease can vary. In general, arthritis can be divided into primary arthritis and secondary arthritis. Primary arthritis includes osteoarthritis and inflammatory arthritides, such as rheumatoid arthritis. Secondary arthritis results from other disorders of the knee, such as prior trauma.
Primary Arthritis
Osteoarthritis of the Knee
Osteoarthritis (OA) of the knee is a common condition characterized by degeneration of the cartilage in one or both knee joints due to wear and tear over time. Osteoarthritis usually develops slowly, resulting in eventual bone-on-bone friction, knee pain, stiffness, and bone spurs in some cases.
Osteoarthritis may be limited to only one “compartment” of the knee. Most commonly, the medial compartment is affected in isolation. When only one compartment is severely arthritic, a partial knee replacement is a consideration for treatment. When two or more compartments are severely arthritic, a total knee replacement is usually the best treatment option.
Inflammatory Arthritis of the Knee
Inflammatory arthritis is a group of autoimmune diseases. These forms of arthritis occur as a result of one’s own immune cells attacking the joint. These diseases may affect multiple or all joints in the body. Types of inflammatory arthritis include:
- Rheumatoid arthritis
- Psoriatic arthritis
- Ankylosing spondylitis
- Juvenile idiopathic arthritis
- Systemic lupus erythematosus
In some patients with these conditions, they develop osteonecrosis of the knee and eventual secondary arthritis as a side effect of disease treatment with chronic and/or high-dose steroids.
Learn more about inflammatory arthritis from hss.edu or arthritis.org.
Secondary Arthritis of the Knee
Secondary arthritis of the knee is a form of arthritis that’s caused by another disease or health condition. Secondary arthritis in the knee may result from:
- Post-traumatic knee arthritis (following a knee injury)
- Skeletal dysplasia
- Knee infection
What Causes Knee Arthritis?
The following conditions can contribute to the onset of knee arthritis:
- Normal aging
- Overuse due to active lifestyle
- Past injury involving the knee joint, such as a meniscus tear, ligament tear, or bone fracture
- Improper joint formation (for example, skeletal dysplasia)
- Malalignment of the leg
- Genetic defects affecting bone or cartilage
- Excess weight
- Other illnesses, causing secondary arthritis
- Metabolic disorders
- Prior knee joint infection
What Are the Signs and Symptoms of Knee Arthritis?
Arthritis of the knee can manifest in different ways, depending on the individual. If you’re experiencing any of the following symptoms, a consultation with an orthopedic knee specialist is recommended:
- Stiffness in the knee, particularly in the morning or after sitting for long periods
- Pain that increases with activity or prolonged standing
- Pain in the knee going up or down stairs
- Pain in front of the knee with kneeling
- Inability to move the knee joint with full range of motion
- Difficulty doing common tasks, such as standing up or bending down
- Pain, soreness, or inflammation/swelling in the knee
- The feeling of bone rubbing against bone (sometimes accompanied by a “crunching” sound or feeling)
- Warmth in the knee that does not go away
- Pain in the knee that wakes you up at night
How Is Knee Arthritis Diagnosed?
Dr. McLawhorn diagnoses knee arthritis with the following methods:
- He will start by asking you a series of questions to better understand your current bone and joint health and your history pertaining to your knee.
- In addition to a medical history, Dr. McLawhorn will conduct a thorough physical evaluation where he will assess your walking, range of motion, and strength around the knee.
- X-rays are an important part of your evaluation to assess the status of your knee joint. If necessary, X-rays of other relevant areas, such as the pelvis, may be ordered for an accurate diagnosis.
- MRI is useful when further examination is needed to determine the health of the bone, cartilage, menisci, or muscles around the knee.
- CT is ordered selectively for patients requiring certain types of knee surgery.
- Blood work or injections into the knee may be necessary for diagnosis in some circumstances.
How Is Knee Arthritis Treated?

Knee arthritis is a progressive condition, and the earlier that it is diagnosed and treated, the more likely it is that you can lessen its impact on your life. In some cases, knee arthritis pain can be well controlled with nonsurgical treatments. Dr. McLawhorn is committed to personalized care for all of his patients, using evidence-based methods and nonsurgical treatment options whenever possible. Nonsurgical treatments for knee arthritis may include:
- Resting
- Avoiding high-impact activities
- Losing weight
- Physical therapy
- Anti-inflammatory medications
- Joint injections
- Using devices to assist in walking, such as a cane
- Knee bracing
When knee arthritis is severe or is not responding well to nonsurgical measures, a surgical procedure may be necessary. Procedures recommended to relieve knee arthritis may include:
- Knee arthroscopy is a minimally invasive surgery often used to address a torn meniscus alongside osteoarthritis. This procedure is particularly effective when the meniscal tear is degenerative and causing noticeable mechanical symptoms, such as painful clicking, catching, or popping in the knee.
- Knee osteotomy is a type of surgery for very young patients with pain and limited arthritis in either the medial or lateral compartment of the knee. In this surgery, the femur (thigh bone) or tibia (shin bone) is surgically broken, and the joint surface is reoriented to improve the alignment of the leg so that the body’s weight is distributed across normal cartilage in the knee. Dr. McLawhorn does not perform this surgery. However, in the rare circumstance that it is required, he will refer patients to a trusted colleague to perform the procedure.
- Partial knee replacement is a surgical procedure involving the removal of the damaged bone and cartilage in one section of the knee joint. The surgeon then positions new artificial components to restore knee function.
- Total knee replacement is a surgical procedure involving the complete replacement of all three compartments of the knee joint with an artificial joint.
Why Choose Dr. McLawhorn?
With offices in New York City and Stamford, CT, Dr. McLawhorn offers accessible, world-class orthopedic solutions. He is renowned for over 600 precise joint replacements each year, using the most advanced techniques, including robotic and minimally invasive surgeries. His expertise in direct anterior total hip replacement has positioned him as a leading figure in joint reconstruction, recognized for his substantial contributions to the field in 2022.
Dr. McLawhorn prioritizes a research-backed, patient-first strategy in every treatment plan. As the Director of Research and Innovation, he is at the forefront of integrating groundbreaking methods that improve recovery and outcomes. You can trust him to give you excellent care and treatment for your knee arthritis.
Frequently Asked Questions
How Long Is the Recovery Period After Knee Surgery?
The recovery period after knee surgery varies depending on the type of surgery performed and the individual patient. Generally, for a total knee replacement, full recovery can take anywhere from three to six months, with most patients resuming light activities within six weeks.
What Can I Do at Home to Manage Knee Arthritis Pain?
Managing knee arthritis pain at home can include several strategies:
- Engage in gentle exercise, such as swimming or walking, to maintain joint function and reduce stiffness.
- Apply heat or cold packs to the knee to relieve pain and inflammation.
- Use over-the-counter pain relievers, such as ibuprofen or acetaminophen, as recommended by your doctor.
- Maintain a healthy weight to reduce stress on the knee joints.
What Kinds of Exercises Help With Knee Arthritis?
Yes, certain exercises can help alleviate symptoms of knee arthritis by strengthening the muscles around the knee, improving flexibility, and reducing joint pain. Effective exercises include:
- Leg raises to strengthen the quadriceps.
- Hamstring stretches.
- Low-impact activities such as cycling or water aerobics.
- Walking to keep the joint moving and increase muscle strength.
These exercises should be performed under the guidance of a physical therapist to ensure they are done correctly and safely.
What Are the Risks of Knee Surgery for Arthritis?
The risks associated with knee surgery for arthritis include infection, blood clots, knee stiffness, and pain. There is also the possibility of implant failure or the need for revision surgery in the future. Discussing these risks with your surgeon can help you understand the potential complications and how they are managed.
How Can I Prevent Knee Arthritis From Worsening?
Preventing knee arthritis from worsening requires a proactive approach. It includes lifestyle changes, proper medical care, and regular monitoring. Here are some practical steps you can take:
- Maintain a Healthy Weight: Excess weight places more strain on the knee joints. This accelerates the wear and tear associated with arthritis.
- Exercise Regularly: Regular low-impact exercises (swimming, cycling, walking, etc.) can help strengthen the muscles around the knee, improve flexibility, and reduce stiffness.
- Avoid High-Impact Activities: Avoiding high-impact activities that put undue stress on the knees, like running or jumping, can prevent further damage.
- Use Supportive Equipment: Supportive footwear and knee braces may also relieve and help protect the joints from additional stress.
If I Have Arthritis in One Knee, Will I Get It in the Other?
Having arthritis in one knee doesn't necessarily mean you'll develop it in the other one. However, the risk can be higher.
Several factors increase the likelihood of developing arthritis in your other knee, including:
- Genetics
- Age
- Lifestyle
- Overcompensation (where you put more stress on the healthy knee to avoid pain in the affected one)
How Can Diet and Nutrition Impact Knee Arthritis Symptoms?
Diet and nutrition can significantly help manage knee arthritis symptoms. Here are some simple adjustments you can make:
- Eat an anti-inflammatory diet rich in fruits, vegetables, whole grains, and lean proteins to reduce inflammation and joint pain.
- Add more omega-3 fatty acids, which are found in fish like salmon and flaxseeds. They are known for their anti-inflammatory properties and can be beneficial in managing arthritis symptoms.
- Maintain a healthy weight through proper nutrition to reduce the strain on knee joints. This is crucial for slowing the progression of arthritis.
- Avoid processed foods, sugars, and saturated fats. These can increase inflammation and exacerbate symptoms.
How Can I Stay Active With Knee Arthritis?
Staying active with knee arthritis is important for maintaining joint flexibility and muscle strength. Focus on:
- Low-Impact Exercise: Low-impact exercises, such as swimming, water aerobics, cycling, and walking, can help keep the joints mobile without causing additional strain.
- Gentle Movement: Gentle stretching and yoga can also improve flexibility and reduce stiffness.
Remember to listen to your body and avoid activities that cause pain or discomfort.
Why Choose Alexander McLawhorn, MD?
Choose Alexander S. McLawhorn, MD, for your knee arthritis treatment and benefit from world-class orthopedic care at the renowned Hospital for Special Surgery.
As a joint reconstruction specialist with offices in New York City and Stamford, Dr. McLawhorn offers personalized, evidence-based treatments tailored to each patient's unique needs. His commitment to shared decision-making ensures compassionate care that aligns with your goals.
Advanced Solutions for Knee Arthritis
If you believe you may be suffering from knee arthritis, it is important to seek advice from an orthopedic knee specialist to accurately diagnose and treat your condition.
Dr. McLawhorn is a hip and knee specialist at Hospital for Special Surgery, serving patients in New York City and Stamford, Connecticut, with extensive training in diagnosing and treating knee arthritis. To learn more, call 203-705-2113 (CT) / 212-606-1065 (NYC) today or schedule an appointment by using the form on this page.



