
If you're struggling with limited mobility, persistent pain, or reduced quality of life due to hip arthritis or other hip conditions, you may be exploring your options for long-term relief. Hip resurfacing is one procedure that can be an effective alternative to total hip replacement surgery in select patients.
Dr. Alexander S. McLawhorn is a board-certified orthopedic surgeon specializing in joint replacement, including advanced hip resurfacing procedures, in New York City and Stamford, Connecticut. With over 600 surgeries performed each year, Dr. McLawhorn is recognized for his expertise in hip preservation techniques and his use of modern technology, including robotic-assisted surgery.
As one of the nation’s leading experts in hip resurfacing, he can help you regain your mobility and quality of life.
What Is Hip Resurfacing?
Hip resurfacing involves removing the damaged portion of the bone and cartilage in the hip socket (acetabulum) and replacing it with a metal shell, after which the ball (femoral head) of the existing joint is resurfaced with a smooth metal covering.
Hip resurfacing is a technically challenging procedure. A successful outcome after hip resurfacing depends on the proper patient, the correct implant with an excellent track record, and having an experienced surgeon like Dr. McLawhorn perform the procedure.


Who Is a Candidate for Hip Resurfacing?
Hip resurfacing is an option for patients with severe hip arthritis that causes pain or limits daily activities. It's most suitable for those with conditions like hip osteoarthritis or hip impingement. It is not designed to correct large bone deformities or significant leg length differences.
The ideal candidate for hip resurfacing typically:
- Is male
- Is under 60 years old
- Has good bone quality (no osteoporosis or bone weakening)
- Has a larger bone size (able to fit a larger implant)
- Has minimal bone deformities or leg length differences
- Has primary osteoarthritis of the hip
Patients with inflammatory arthritis, such as rheumatoid arthritis, are generally not candidates.
Women are also not usually candidates, especially those of childbearing age. This is because of their smaller bone structure and the risk of metal ions affecting pregnancy or causing reactions around the hip joint.
When Should I Consider Hip Resurfacing Surgery?
When your hip pain begins to interfere with your daily life, prevents you from participating in your recreational activities, wakes you from sleep, and/or requires prescription pain medication, it may be time to consider hip surgery of some sort.
Dr. McLawhorn favors hip resurfacing vs. total hip replacement in younger male patients with primary hip osteoarthritis who intend to participate in activities with a lot of running or impact on the hip.
That said, choosing to have a hip resurfacing surgery is a personal decision. Your preference for surgery, your lifestyle demands, and your expectations for outcomes after surgery aid the decision-making process and will guide your choice between nonsurgical care and hip surgery. Dr. McLawhorn is happy to help you make your decision in any way he can.
What Are the Goals for Hip Resurfacing Surgery?
First and foremost, the purpose of hip resurfacing surgery is to improve pain. Other general goals are to:
- Improve hip function
- Provide a stable hip that does not dislocate
- Prevent excessive wear of the implanted components
- Avoid complications
What to Expect During Hip Resurfacing Surgery
Hip resurfacing, like total hip replacement, involves removing damaged cartilage and bone from the hip socket, but Dr. McLawhorn preserves more of your natural bone by reshaping the femoral head and capping it with a smooth metal covering.
Here’s how he performs the procedure:
- You’ll first receive regional anesthesia (spinal or epidural) to numb your lower body and sedation to sleep through the surgery. You will also receive antibiotics before to prevent infection.
- To begin the surgery, Dr. McLawhorn makes an incision to access the hip joint and carefully dislocates the hip.
- He removes the damaged cartilage, reshapes the hip socket, and places the metal shell inside.
- The femoral head is reshaped and capped with a metal covering.
- Dr. McLawhorn then reassembles the joint and closes the soft tissues over the hip.
Recovery After Hip Resurfacing
Recovering from hip resurfacing is a gradual process. Below are some important aspects and timelines:
- Walking: You’ll be able to walk with crutches right after the procedure. Crutches are typically needed for a few weeks while your bone adjusts to the implant.
- Precautions: For about six weeks, avoid crossing your operated leg, turning it inward, or bending it more than ninety degrees.
- Return to work: Depending on your job, you may be able to return to work within two to three weeks.
- Full recovery: Expect to resume normal activities, including sports and heavy labor, in about six months.
- Follow-Up Care: Regular check-ups with Dr. McLawhorn will be scheduled at six weeks, twelve weeks, one year, and then every one to two years to monitor your progress with exams and X-rays. Ultrasound and/or MRI tests are not necessary for routine patient visits.
Ideally, you’ll be able to go back to work and the activities you love to perform without worrying about your hip resurfacing. After complete recovery from surgery, some patients even forget that they had hip surgery.
What Materials Are Hip Resurfacings Made Of?
Dr. McLawhorn uses the Birmingham Hip Resurfacing (BHR) implant, which has one of the best success rates in the U.S., the U.K., and Australia. It has a low risk of complications and often lasts longer than a total hip replacement for the right patients.
The implant is made of strong cobalt-chrome metal and consists of these parts:
- Metal shell: This is press-fit into the reshaped hip socket (acetabulum). The outer surface is coated with a special material (hydroxyapatite) that helps your bone grow onto it, securing it in place over time.
- Metal femoral head: This caps the reshaped ball of the hip joint and is attached with bone cement for stability.
Both the shell and head are polished to create low-friction movement that reduces wear and tear.
What Are the Advantages of Hip Resurfacing?
The advantages of hip resurfacing surgery compared to total hip replacement are:
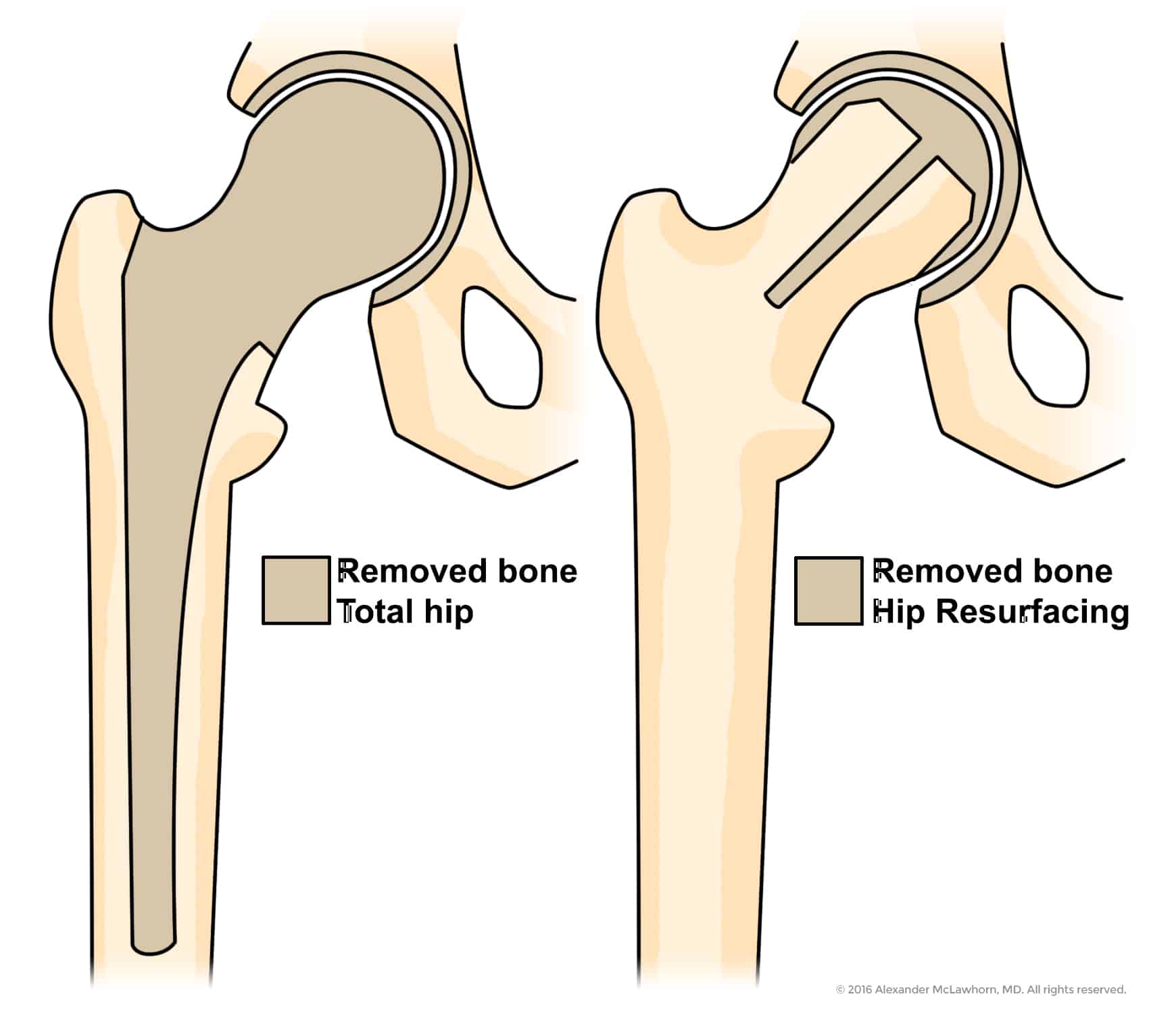
- Preserving more bone: Unlike a total hip replacement, hip resurfacing retains more of the natural bone in your thigh. This can be especially helpful for younger patients who might need future hip surgeries.
- Larger femoral head: After hip resurfacing, the size of the femoral head (the ball of the hip joint) is larger and closer to the natural size of your hip. This can improve your range of motion and reduce the risk of hip dislocation compared to a total hip replacement. This can be important to patients who need a higher range of motion for work or sports.
What Are the Risks of Hip Resurfacing?
Hip resurfacing has shown excellent results for the right patients, with many experiencing long-term success. However, like any surgery, there are some risks to be aware of:
- Femoral neck fracture (occurs in about 1% of patients): This is a break in the bone just below the resurfaced hip joint. If it happens, another surgery might be needed to convert the hip resurfacing to a full hip replacement.
- Soft tissue reactions: In rare cases, some patients may develop reactions around the hip joint (called ALTR), which could cause discomfort or swelling.
- Elevated metal ions: Some patients with metal-on-metal implants may have higher levels of cobalt and chromium in their blood. We monitor this with regular testing, and if there are no symptoms, you may not need treatment.
- Loosening of the implant: In a small number of cases, the components of the resurfacing may loosen over time, but this is uncommon.
It's important to remember that while these risks exist, they are rare. Regular check-ups and monitoring will help ensure that everything is functioning well. Even in successful hip resurfacings, low levels of metal ions are usually detected, but the long-term effects of these small amounts are not fully known.
How Can I Prepare for My Hip Resurfacing Procedure?
To prepare for your hip resurfacing, we recommend patients to the following:
- Ask about your medications: Consult your primary doctor about stopping any medications that may affect your recovery or your body’s reaction to surgery.
- Arrange transportation: Designate a friend or loved one to you to and from your appointment.
- Prepare your home: Place frequently used objects closer to your resting area in your home until you can walk free of pain. You might even move your bed from the second floor to the first floor to avoid walking upstairs in your first few weeks of healing.
- Quit smoking: Smoking can block your body from getting the nutrients it needs to heal from operations, so it’s best to stop smoking.
- Eat a balanced diet: Maintaining a stable weight will help your body stabilize carrying your weight on your hips. Eating healthy can help you avoid excessive weight gain, eliminating the need for stronger pressure.
- Stick to a light exercise routine: Slow walking and light stretching will help you slowly get comfortable with movement after your surgery. This can also help you maintain a stable weight during your recovery period.
How Long Will the Results From My Hip Resurfacing Procedure Last?
Contemporary hip resurfacing implants have been used for over 20 years. Approximately 90% are still doing well at the 20-year mark.
Keep in mind that the implants used in hip resurfacings are mechanical devices and may fail over time for various reasons, including bearing wear, loosening, infection, fracture, and dislocation. Routine surveillance of hip resurfacing implants is recommended at regular intervals to evaluate X-rays and blood metal ions.
How Do I Know if I Need Hip Resurfacing or Total Replacement?
Deciding between hip resurfacing and a total hip replacement depends on your age, activity level, and the condition of your hip.
- Hip Resurfacing is often a better option for younger, active patients who want to preserve more of their natural bone and expect to continue high-impact activities like running or sports. It’s typically recommended for men under 60 with good bone quality.
- Total Hip Replacement is usually the better choice for older patients, those with more severe bone damage or deformities, or individuals with conditions like rheumatoid arthritis.
Dr. McLawhorn will help guide you through this decision based on your specific situation.
The Importance of Post-Surgery Rehabilitation
Recovering from hip resurfacing surgery doesn’t end when you leave the operating room. You need consistent physical therapy and rehabilitation efforts in order to regain full mobility and strength in your hip. Dr. McLawhorn and his team will work closely with you to develop a plan that supports your recovery at each stage.
During the first few weeks after surgery, your physical therapy will focus on gentle movements to help improve your range of motion while protecting the healing joint. As your recovery progresses, therapy will shift to strengthening the muscles around your hip, helping to restore balance and stability.
In the long term, sticking with your rehabilitation program helps reduce the risk of complications and helps you get back to normal life. Patients who actively engage in physical therapy often experience faster recovery times, increased mobility, and better long-term results.
Why Choose Alexander S. McLawhorn, MD?
Dr. Alexander S. McLawhorn is a board-certified orthopedic surgeon and one of the nation’s leading experts in hip resurfacing and joint replacement. Performing over 600 joint surgeries each year, including more than 400 robot-assisted hip replacements annually, Dr. McLawhorn’s experience and precision in advanced surgical techniques set him above the rest. As the top surgeon by volume at the Hospital for Special Surgery (HSS), he consistently delivers exceptional outcomes for his patients.
Dr. McLawhorn is also the Director of Research and Innovation for the Adult Reconstruction and Joint Replacement Service at HSS. He has been recognized with numerous prestigious awards, including the Frank Stinchfield Award from the Hip Society, and continues to lead research that improves the value of joint replacement surgeries across the country. At the end of the day, Dr. McLawhorn’s goal is simple: to help his patients recover faster and stay active longer.
Learn More About Hip Resurfacing in NYC and Stamford
If you are suffering from a debilitating hip condition and exploring hip resurfacing as a treatment option, talk to orthopedic hip specialist Dr. Alexander McLawhorn to accurately diagnose and treat your condition.
Dr. McLawhorn serves patients at Hospital for Special Surgery facilities in New York City and Stamford, Connecticut. To learn more, call 203-705-2113 (CT) / 212-606-1065 (NYC) today or schedule an appointment online.
Learn more about what you can expect before and after surgery in Dr. McLawhorn’s FAQs.



