When joint pain starts to limit how you move, work, or sleep, it’s time to explore your options.
Dr. Alexander McLawhorn is a board-certified orthopedic surgeon specializing in advanced hip and knee procedures in New York City and Stamford, Connecticut. He brings specialized expertise in hip and knee surgery, with a strong emphasis on research-driven techniques that improve long-term outcomes.
Click on the buttons below to learn more about the procedures performed by Dr. McLawhorn.
Total Hip Replacement
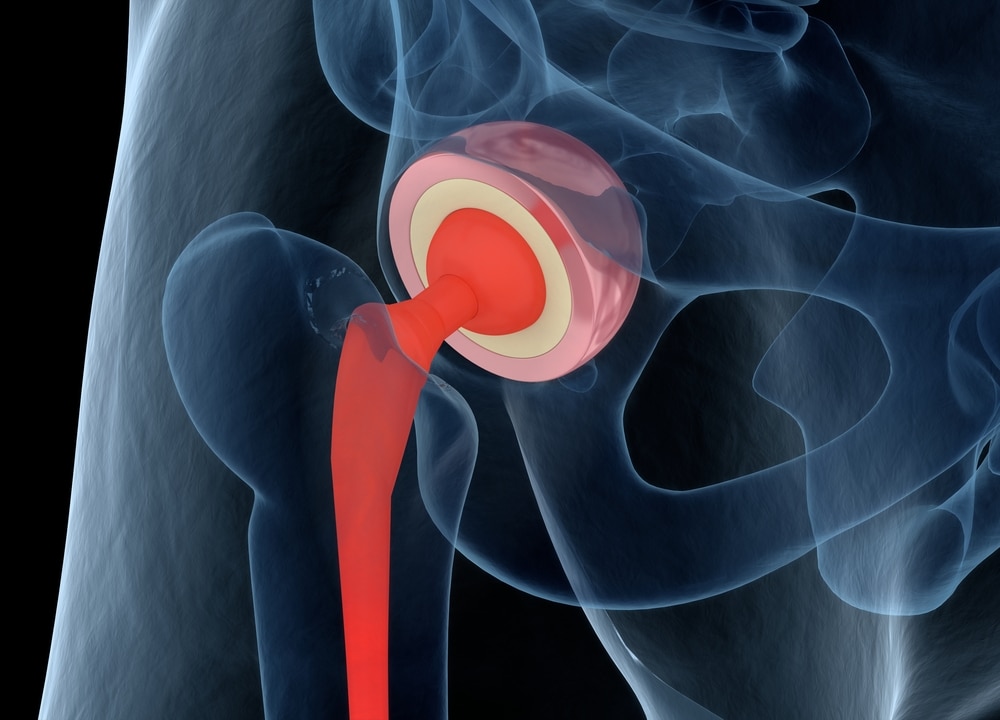
If hip pain has started limiting your movement or making daily activities more difficult, a total hip replacement could help you feel like yourself again. This procedure replaces the damaged ball-and-socket joint with smooth, long-lasting implants.
Dr. McLawhorn typically uses the anterior approach, which avoids cutting through muscle. Most people can walk the same day as surgery, return to regular activities within a few months, and enjoy a more active lifestyle again without the distraction of constant joint pain.
Bikini Hip Replacement
Bikini hip replacement is a variation of the anterior approach that uses a horizontal incision along the groin crease for a more discreet scar. It offers the same muscle-sparing benefits as traditional anterior hip replacement but with improved cosmetic healing.
Dr. McLawhorn performs this procedure for eligible patients who want less visible scarring without compromising recovery.
Hip Resurfacing
Hip resurfacing can often be the right fit for younger people who are still active but struggle with hip pain. Instead of removing the entire joint, Dr. McLawhorn reshapes and caps the ball of your hip with a metal covering while replacing the damaged socket.
This option preserves more of your natural bone and is often better for high-impact movement, especially in men under 60 with strong bone quality. Recovery takes time, but many patients return to sports or physical work without having to worry about the stability of their joints.
Total Knee Replacement
When pain, stiffness, or swelling in your knee won’t go away and conservative treatments stop working, total knee replacement may be your next step. This surgery replaces the worn-out surfaces of your knee with metal and plastic implants that restore smoother motion.
Dr. McLawhorn focuses on getting your new knee aligned and stable so you can walk more comfortably, regain strength, and get back to the things you enjoy. Recovery can take up to a year, but you'll likely start to notice major improvements within a few months.
Partial Knee Replacement
A partial knee replacement is a less invasive option when knee pain is isolated to one area (often the inside part of the knee). Instead of replacing the whole joint, Dr. McLawhorn removes only the damaged section and resurfaces it with a compact implant.
You keep more of your natural bone, your ligaments stay intact, and your knee often feels more “normal” after healing. Recovery is typically quicker than a full replacement, and you can typically go home the same day as surgery.
Robotic and Computer-Assisted Joint Replacement
For even greater accuracy during surgery, Dr. McLawhorn often uses computer-assisted or robotic-guided technology. These tools don’t perform the surgery, but they do help guide it.
With real-time imaging and precision feedback, your implant can be positioned more accurately, which helps it last longer and work better. This technology helps reduce the risk of complications and supports a smoother recovery.
Common Joint Problems
Hip and knee joints take on a lot of daily stress, which makes them especially vulnerable to damage over time. When these joints become worn down or injured, even simple movements like walking, bending, or climbing stairs can become painful or difficult.
Some of the most common issues that lead people to consider orthopedic care include:
- Osteoarthritis: The most frequent cause of joint pain, osteoarthritis gradually wears away the cartilage that cushions your hip or knee joints. As the cartilage thins, bones can grind against each other, leading to ongoing discomfort, especially with movement.
- Previous Injuries: Injuries like fractures, ligament tears, or dislocations can alter the way your joint moves and functions. Even after healing, these injuries can lead to long-term instability or early-onset arthritis.
- Degenerative Joint Conditions: Conditions such as avascular necrosis or post-traumatic arthritis cause the bone and cartilage within the joint to deteriorate. These problems often progress despite rest or conservative treatment and may eventually require surgical correction.
- Hip Dysplasia and Childhood Hip Disorders: Some joint problems begin earlier in life. Conditions like hip dysplasia or developmental disorders can lead to misalignment, joint damage, or early arthritis that worsens with age and activity.
- Reduced Range of Motion and Stiffness: Limited flexibility, joint locking, or persistent stiffness can interfere with your ability to move comfortably. These symptoms may worsen over time, making daily activities like standing, sitting, or getting in and out of a car increasingly difficult.
Why Choose Dr. Alexander McLawhorn?
With over 600 joint replacements performed each year, Dr. Alexander McLawhorn ranks among the most experienced hip and knee surgeons in the country. He serves as Director of Research and Innovation for the Adult Reconstruction and Joint Replacement Service at the Hospital for Special Surgery (HSS) – a national leader in orthopedics.
Patients trust Dr. McLawhorn for his clear explanations and results-driven approach. He assesses your lifestyle, anatomy, and long-term goals to help you decide on the right procedure. Backed by extensive clinical research, he prioritizes faster recovery, improved joint function, and durable results.
Frequently Asked Questions
How Are Joint Problems Diagnosed and Planned for Surgery?
Dr. McLawhorn uses imaging tools like X-rays, MRIs, and CT scans to evaluate joint damage, alignment, and bone quality. These tests help confirm the source of your pain and guide treatment decisions.
For joint replacements, 3D mapping and planning software may be used to customize implant size and positioning. This approach improves accuracy in surgery and supports better function of the new joint.
How Long Do Implants Last?
Joint replacement implants are designed to be durable, with most lasting 15 to 20 years or longer, depending on your activity level, weight, and health.
While many people enjoy long-term relief with no further intervention, implants can wear down or loosen over time. In some cases, a revision surgery may be needed to replace or adjust the components, especially if there’s pain, instability, or changes seen on imaging.
Regular follow-up visits help monitor the condition of your implant and catch any issues early.
Is Joint Replacement Surgery Safe?
Yes, joint replacement surgery is considered very safe when performed by an experienced surgeon. Dr. McLawhorn uses advanced techniques and evidence-based protocols to reduce the risk of complications.
What Type of Implants Will I Receive?
Implants are selected based on your anatomy, activity level, and bone quality. Dr. McLawhorn uses high-quality components with proven durability, often incorporating materials like titanium, cobalt-chrome, and polyethylene.
How Is Pain Managed After Surgery?
Pain management is a key part of the surgical plan and begins before your procedure even starts. Dr. McLawhorn uses multiple strategies that may include:
- Regional anesthesia to numb the lower body during surgery
- Nerve blocks to reduce pain in the first 24–48 hours after surgery
- Personalized medication plans based on your needs and health history
- Minimally invasive techniques that limit tissue disruption and promote early mobility
Most patients are able to stand or walk on the day of surgery with much less pain than they expect.
How Should I Prepare for a Consultation?
To make the most of your visit, it’s helpful to bring any recent imaging (such as X-rays, MRIs, or CT scans) as well as medical records related to your joint condition. A current list of medications, including supplements, is also important. Be prepared to discuss your symptoms in detail, including when they began, what makes them better or worse, and how they affect your daily activities.
Wearing comfortable, loose-fitting clothing can make it easier for Dr. McLawhorn to examine your hip or knee. You may also want to jot down any questions you have about treatment.
What Questions Should I Ask Dr. McLawhorn?
Here are some important topics to consider discussing during your consultation:
- What is the exact cause of my hip or knee pain?
- Which procedure do you recommend, and why?
- How long will the implant last in my case?
- What kind of anesthesia will I receive?
- How long is the typical recovery timeline?
- When can I return to work, driving, or physical activity?
- Will I need physical therapy after surgery?
- What happens if I delay surgery?
These questions can help guide your decision-making and give you a clearer picture of what to expect before, during, and after surgery.
Trusted Orthopedic Care in NYC & Stamford
If you're ready to stop letting joint pain control your life, you're in the right place. With thousands of successful procedures and locations in both New York City and Stamford, Dr. McLawhorn offers the precision, experience, and support you need to move forward.
Call 212-606-1065 for NYC or 203-705-2113 for Stamford to schedule your consultation today.








